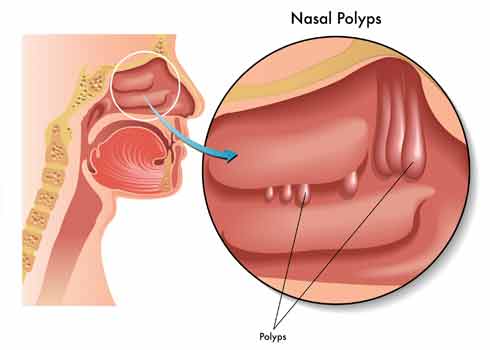
Nasal Polyps
Introduction
Nasal polyps are swellings of the normal nasal lining that occur inside the nasal passages and sinuses.
They are typically pearly in colour and can vary in size. Each polyp is teardrop-shaped, and can look like a grape when fully grown.
You may not always know if you have nasal polyps because they can be difficult to see and don't always cause any symptoms.
What problems can they cause?
Nasal polyps usually only cause problems if they are large or grow in clusters.
Symptoms can include:
-
a blocked nose, which can make it difficult to breathe through your nose
-
a runny nose
-
mucus that drips from the back of your nose down your throat (post-nasal drip)
-
a reduced sense of smell or taste
-
a feeling of fullness or pressure in the face
-
snoring
-
obstructive sleep apnoea (OSA) – your airways become temporarily blocked while you're asleep, which can disturb your sleep
If polyps block your sinuses, they can cause a build-up of fluid that may become infected (sinusitis). If this happens, you may have facial pain,toothache and fever.
When to see your ENT doctor?
The symptoms of nasal polyps can be very similar to those of more common conditions, such as a cold. However, colds tend to clear up within a few days, whereas nasal polyps usually won't get better unless they're treated.
You should see your ENT doctor if you have nasal symptoms that last a month or more.
What causes nasal polyps?
Nasal polyps are thought to develop as a result of inflammation of the lining of the nasal passages and sinuses. The lining becomes increasingly swollen and then hangs down.
It's unclear exactly what triggers this inflammation, although certain things can increase your risk of developing nasal polyps, including:
-
asthma– 20-40% of people with nasal polyps also have asthma
-
aspirin intolerance – allergy-like symptoms, such as a watery nose, occur if you take aspirin or other non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen
Nasal polyps usually affect adults and are more common in men than women. They're rare in children.
Diagnosing nasal polyps
Your ENT doctor will ask you about your symptoms and examine the inside of your nose.
Usually a nasal endoscopy will often be needed to confirm polyps and to determine how large they are . If nasal polyps are diagnosed usually you will need a CT scan to evaluate their extend.
Treating nasal polyps
Nasal polyps can be difficult to get rid of permanently, but steroid medication can often help shrink them, and surgery to remove them can be carried out if medication doesn't help.
The main treatments are:
-
corticosteroid nose drops or nasal sprays to shrink the polyps over a number of weeks or months
-
corticosteroid tablets to shrink larger or more troublesome polyps quickly, although they're not usually used for more than 10 days because of the risk of side effects
-
surgery to remove large or persistent polyps using tiny surgical instruments inserted up your nostrils
As polyps can grow back after treatment, including after surgery, you will usually be advised to continue using corticosteroid nasal sprays to help stop them returning quickly.
Surgery
Surgery to remove nasal polyps may be recommended if steroid medication doesn't help or your polyps are particularly large.
The procedure to remove nasal polyps is called functional endoscopic sinus surgery (F.E.S.S). It's carried out under general anaesthetic, sometimes as a day procedure.
The surgeon will pass an endoscope (a tube with a video camera at one end) into your nostrils to allow them to see inside your nose and sinuses.
Surgical instruments, such as a micro-debrider (a tiny motorised revolving shaver) are passed up your nostrils and used to remove the polyps. This means it's not necessary to make any cuts to your face.
You will usually be advised to rest for around two weeks after surgery. Your surgeon will be able to give you more detailed information and advice.
Long-term use of steroid nasal spray will usually be recommended after surgery to help stop polyps returning quickly.